The Clinical Classroom
Saint Joseph’s Center for Excellence in Practice (CEP) has nursing and allied health students tackling high-stress healthcare scenarios within the safety of a simulation.
By Emmalee Eckstein
Walk through the sprawling hallways of Saint Joseph’s new Lancaster location and you’ll find high-fidelity manikin and patient-actor simulation experiences, replica ICU beds and operating rooms, ultrasound and respiratory care labs, and even a fully staged apartment where students practice home-care skills.
The state-of-the-art Center for Excellence in Practice (CEP) features 20,000 square feet of immersive simulation space that aids students in the School of Nursing and Allied Health to build real-world skills in a safe environment.
“Even in their rotations, students don’t get to make independent clinical decisions,” explains Kristen Zulkosky, PhD, RN, CNE, CHSE, clinical professor of nursing, who oversees nurse education with the simulators. “They’re either checking back with their primary nurse or a faculty member — they don’t get experience calling any shots. In the CEP, they’re in charge. They’re thinking on their feet and learning from their mistakes directly and safely.”
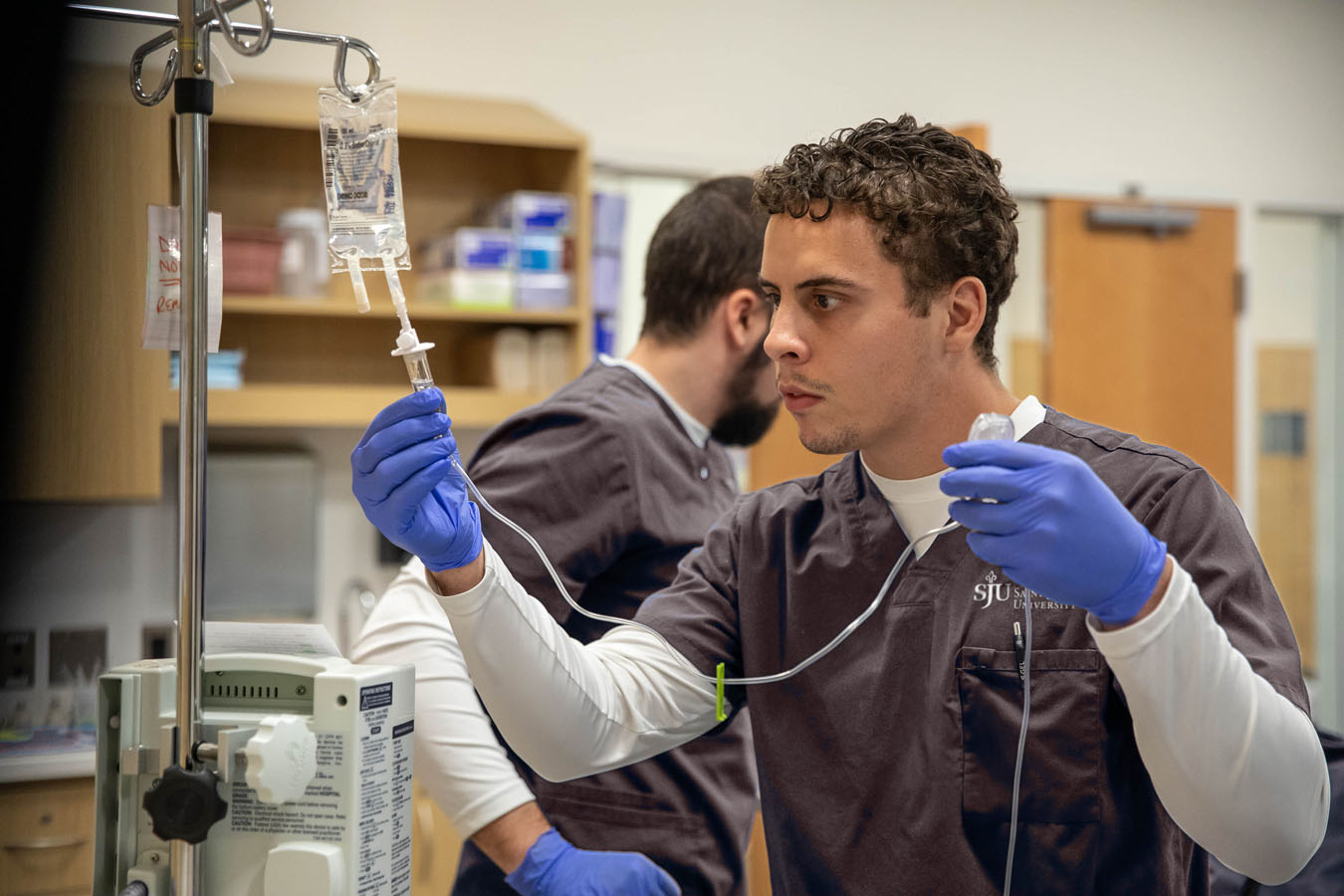
To make this experience possible, the CEP is furnished with top-of-the-line technologies to give students a chance to get comfortable within real-world hospital settings.
“The CEP is a great place to teach healthcare because students can practice skills in all health specialties in one spot. Healthcare education can sometimes happen in silos, so having students work next to each other to experience different health specialties can help them better understand each other's roles before they've even set foot in the hospital,” says Nicholai Best, the CEP’s nursing simulation operations manager. “The facility is also made to look like a real hospital, so students feel like they’re learning inside of an actual healthcare setting, not just a classroom.”
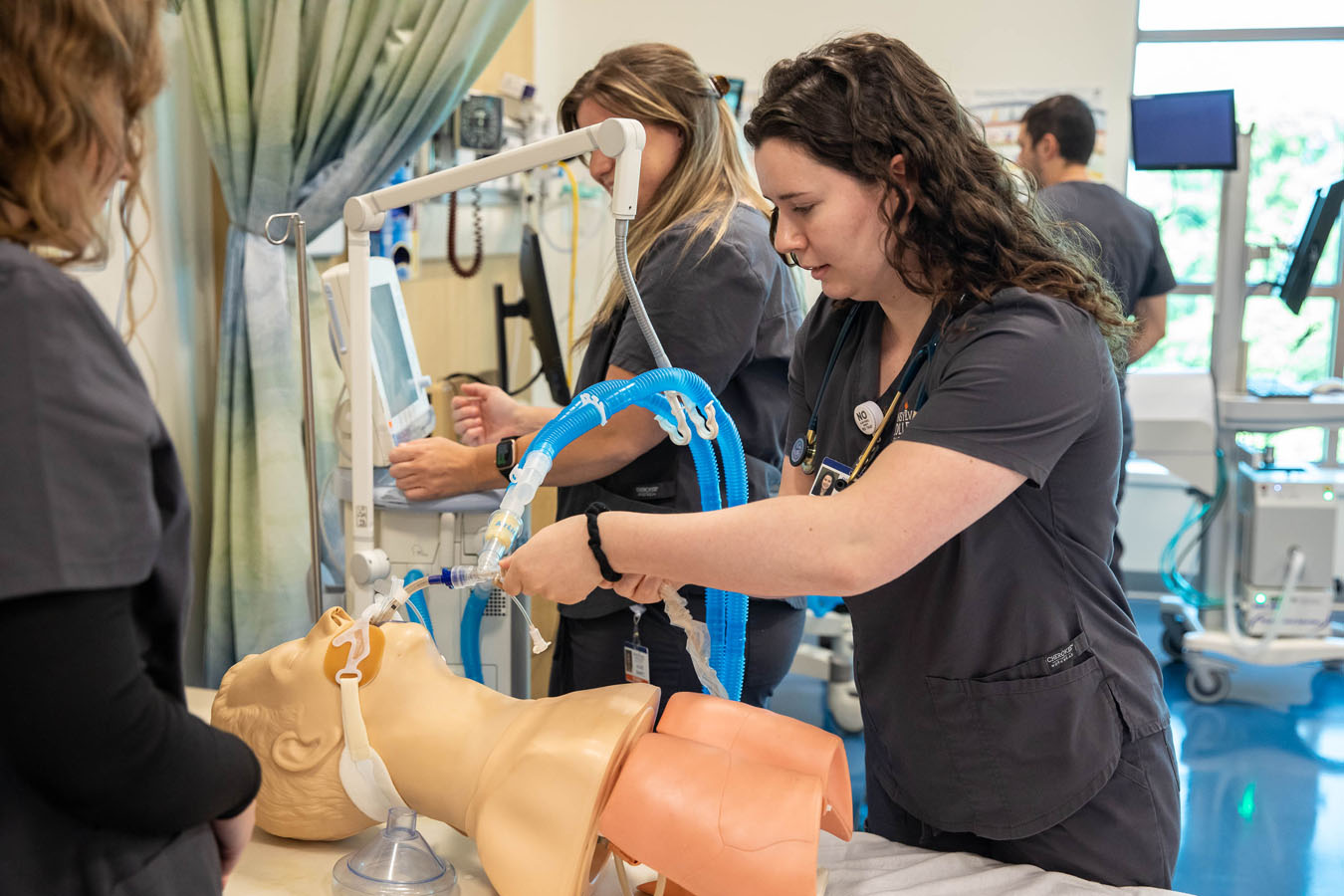
Patient Simulators
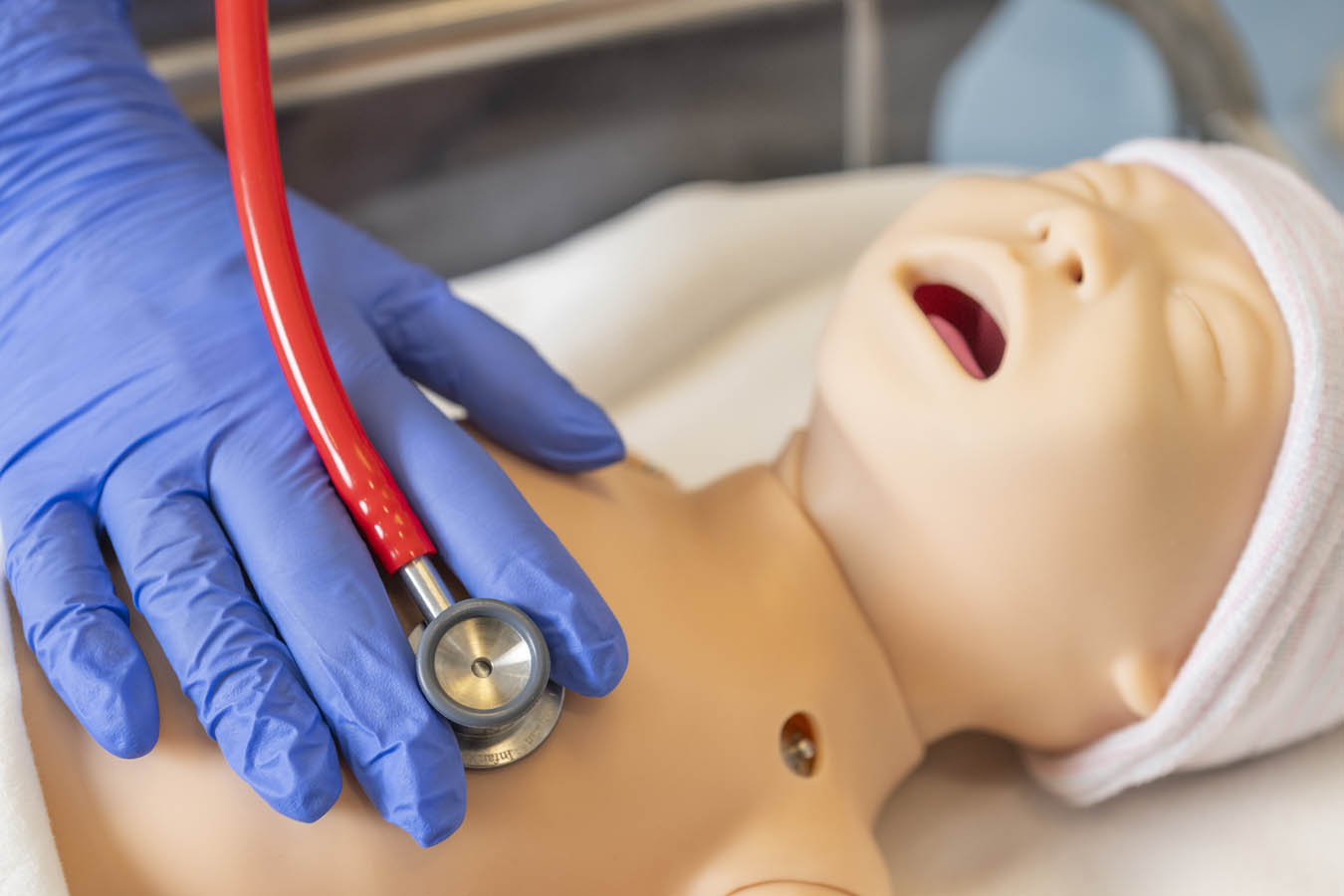
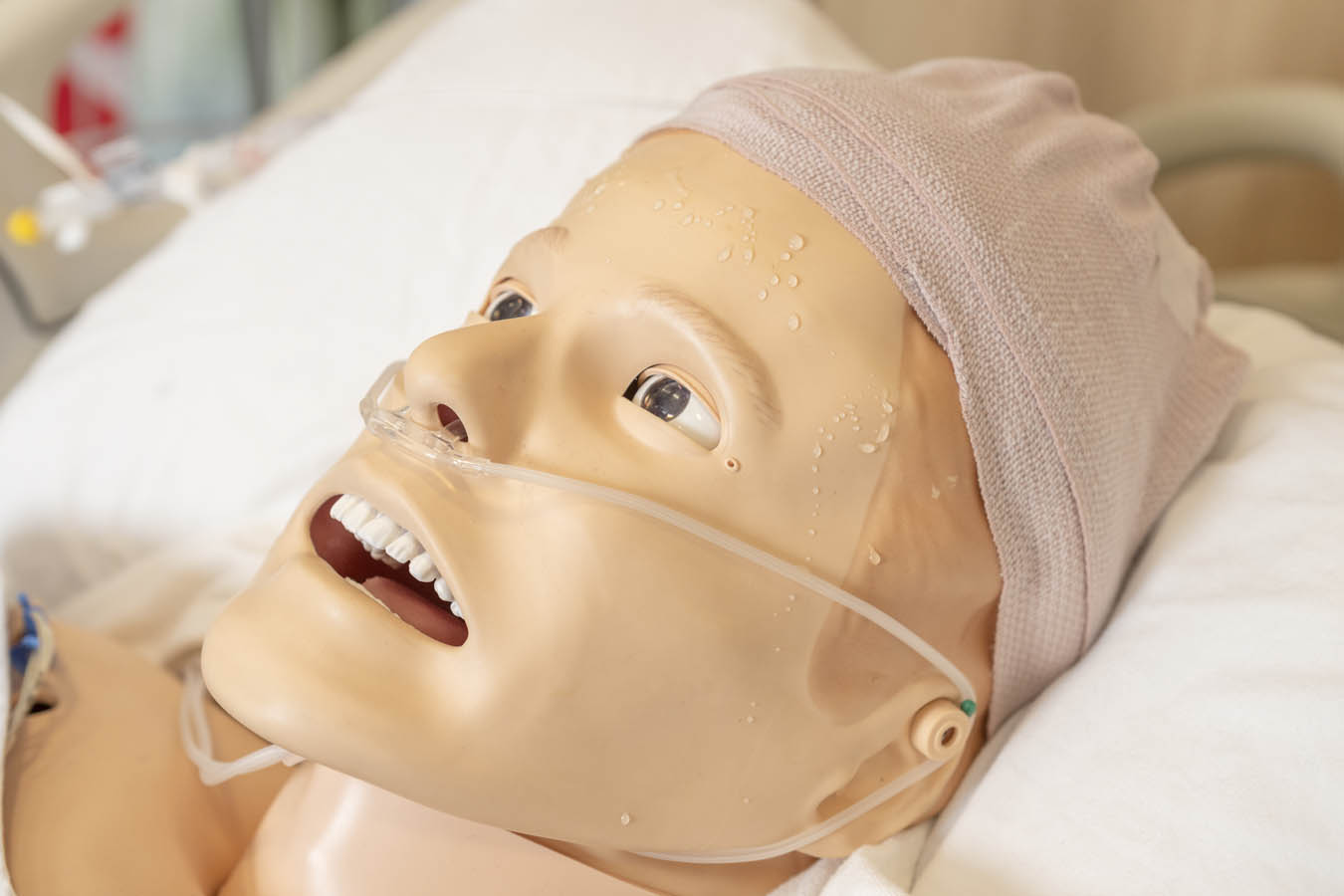
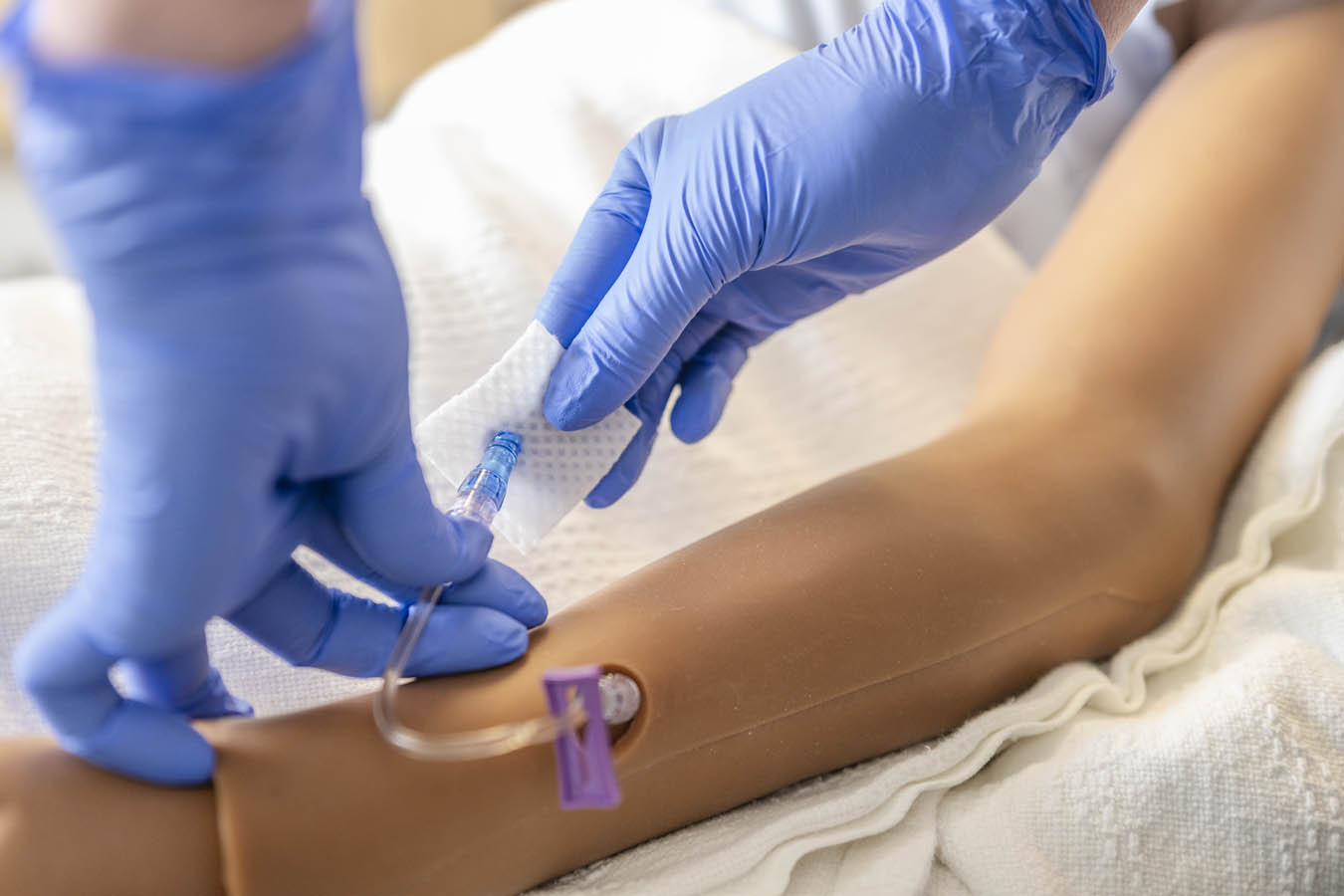
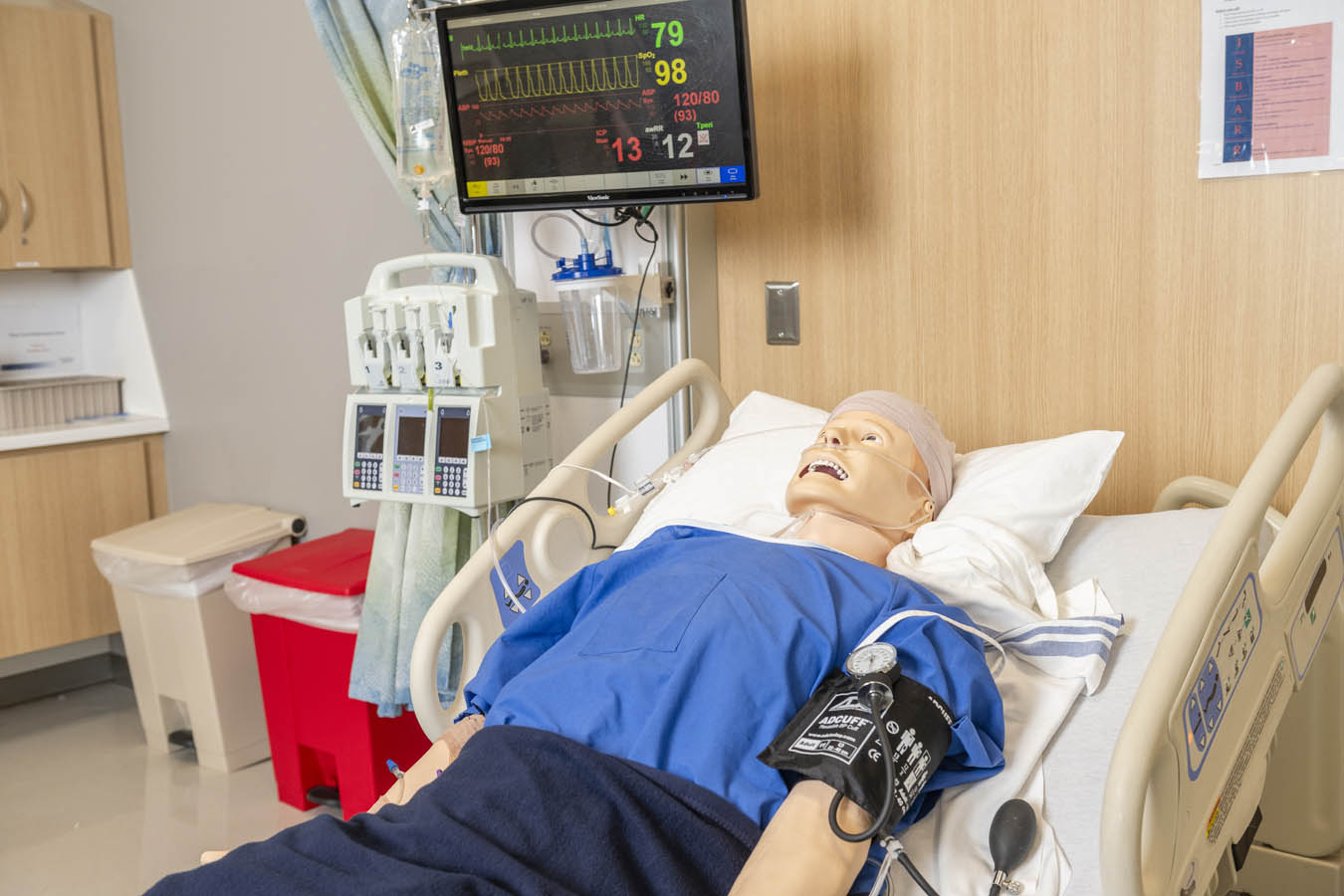
The CEP’s high-fidelity manikins can blink, cry and sweat — some of them even have reactive pupils. On these simulators, students practice urinary catheterization, listen for heart and lung sounds, and more. But a flat manikin can’t put on a show. And that’s where the simulated patients or patient actors come in.
“To run a really good mental health scenario, we need real people,” says Zulkosky. “We create scenarios where the simulated patients are agitated, pacing, in very clear distress — it really brings the situation to life for our students.”
Patient actors are provided with scripts and directions that can take students through an unfolding, multi-day health crisis within the course of their eight-hour clinical rotation. Students may start with the simulation in the CEP’s home-care apartment, then travel to the multi-patient nursing unit and, finally, end up in the ICU. These unfolding scenarios are often captured via video so students are able to review the footage and learn from mistakes or highlight areas of accomplishment.
The CEP also has SonoSim technology, which is software that can be used in diagnostic medicine to show students abnormal images via ultrasound. With this tool, students scan a manikin that has a blocked carotid artery or an abnormal fetal measurement, which likely wouldn’t be viewable on an everyday human volunteer.
Multi-Patient Nursing Unit
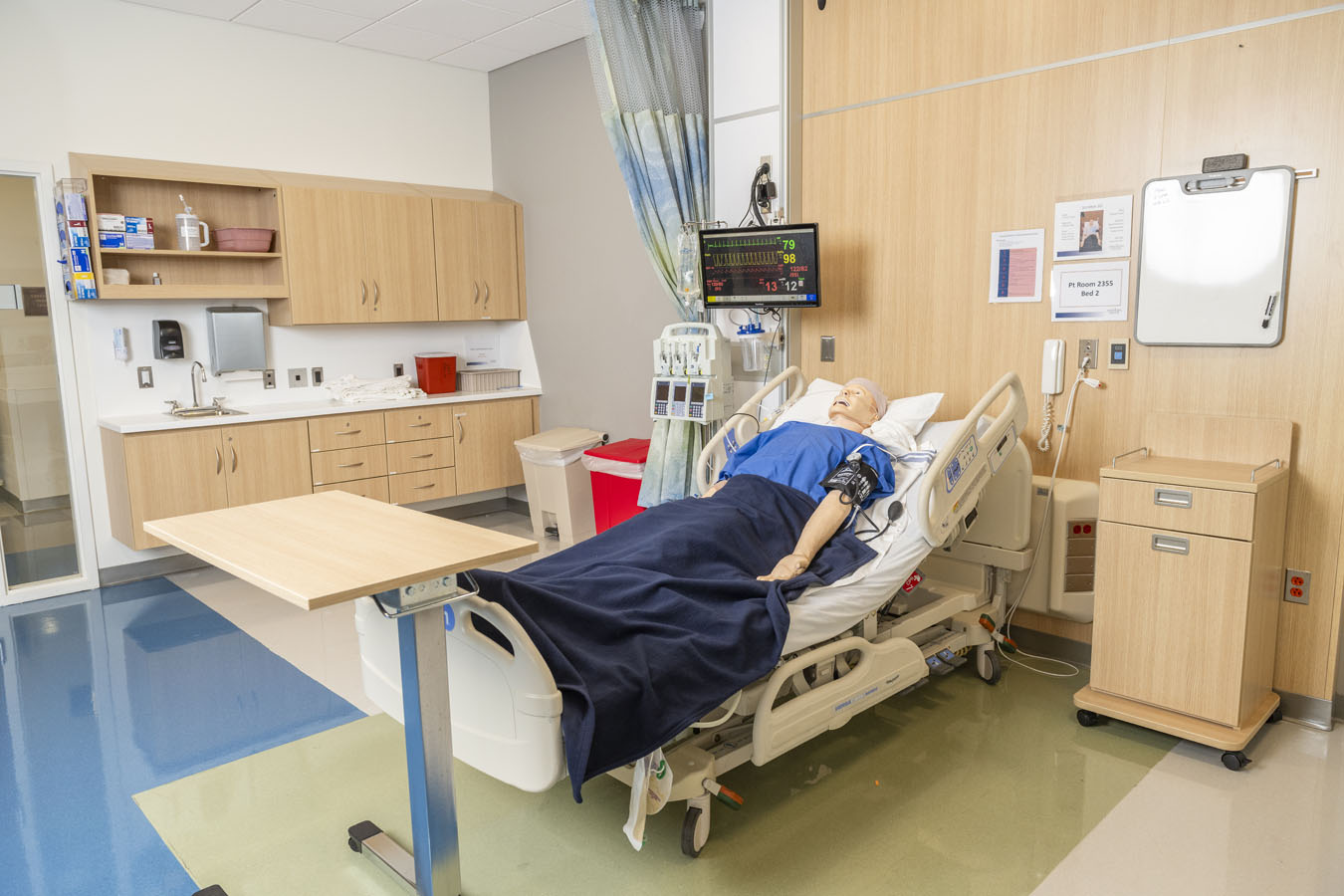
The multi-patient nursing unit was designed to provide the feel and functionality of a real in-patient clinical environment for Saint Joseph’s nursing students. This area has a central nurses station and four single patient rooms, which are connected for seamless patient care.
This unit includes telemetry monitoring, a nurse-call system with a “code blue” alarm (a hospital alert signifying any patient with an unexpected cardiac or respiratory arrest requiring resuscitation and activation), a central medication preparation area, documentation stations, a crash cart and more. All these tools make it possible for instructors to assess students’ time-management skills, as well as their ability to delegate tasks and to think critically on their feet while managing and evaluating multiple patients.
Intensive Care Unit (ICU)
Across the hall from the multi-patient unit are the two ICU rooms that hold two beds each. These large rooms can either accommodate more students or more equipment to care for critically ill patients. The rooms can also be used to hold small teaching sessions.
Each room can be viewed with a camera system or can be observed directly from the control room via one-way glass.
This setup allows students to practice independently without their instructor’s aid. The camera system is also used for other students to observe simulations remotely in a debriefing room within CEP.
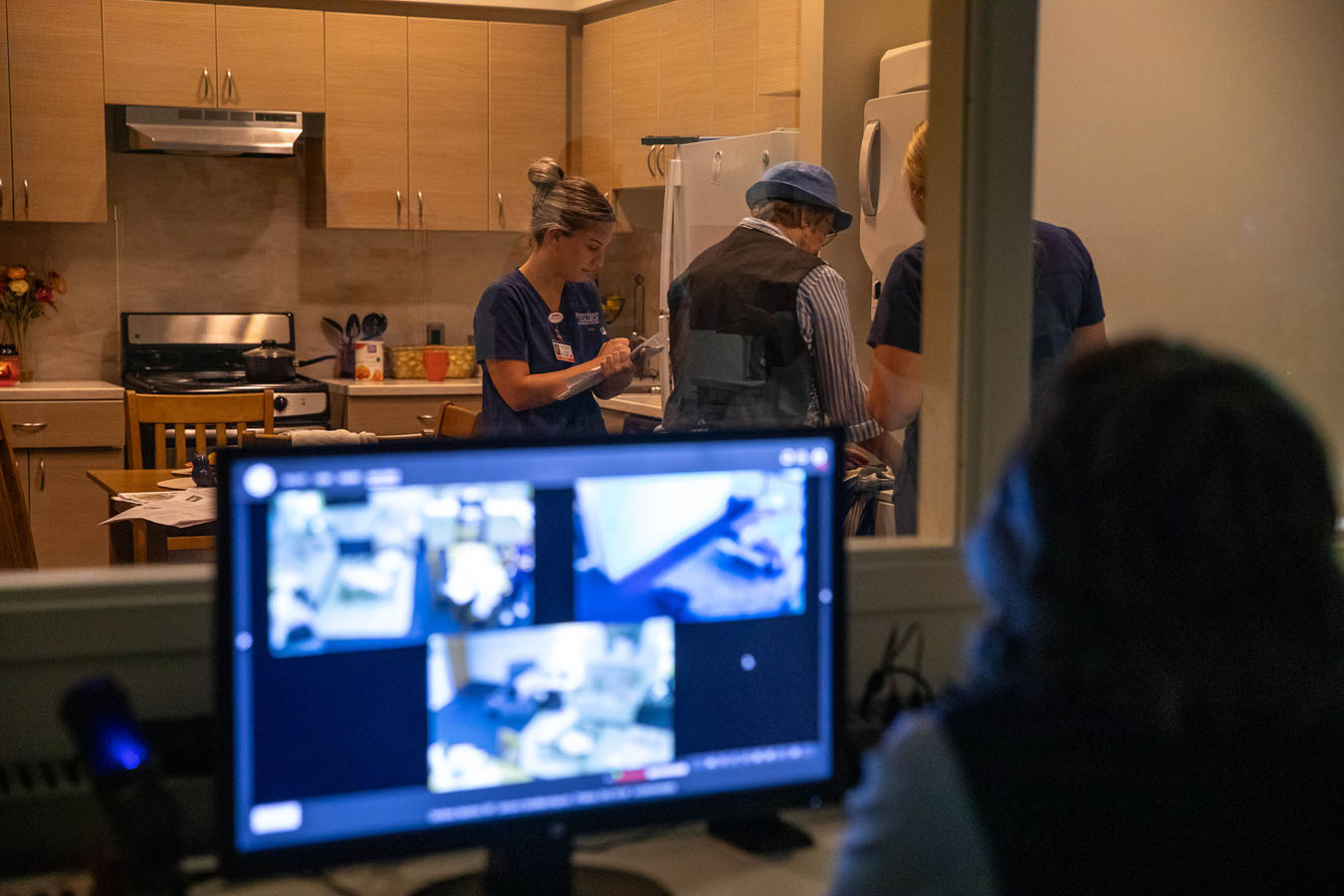
Home-Care Apartment
Designed and furnished to replicate a studio apartment, this unit was created with visiting nurses and emergency medical services in mind. The staged apartment includes a living room, fully equipped kitchen, dining area, bedroom and a functional bathroom with a full tub. With the exception of the bathroom, the entire apartment can be viewed by camera or via one-way glass.
Here, students are taken through healthcare situations that may happen at home, like hospice or death and dying scenarios; they assess untenable living situations and make sure a home environment is free from dangers such as tripping hazards and faulty smoke detectors. Actors are often used to educate students in the home-care apartment, bringing to life the humanity of these painful situations.
“In the end-of-life scenario, we have an actor who portrays the wife of a patient who dies right there in the apartment bed. It prepares our students to handle that situation with care,” says Best. “Students don’t often get the chance to experience navigating that grief process until they are in the thick of it. This simulation provides them with practice and tools they can use to interact with grieving family members compassionately and considerately.”
Respiratory Therapy Lab
There are two respiratory therapy labs in the CEP, configured with three patient beds and four headwalls in each lab, an intentional design allowing for easy instruction and interaction at an adjacent table.
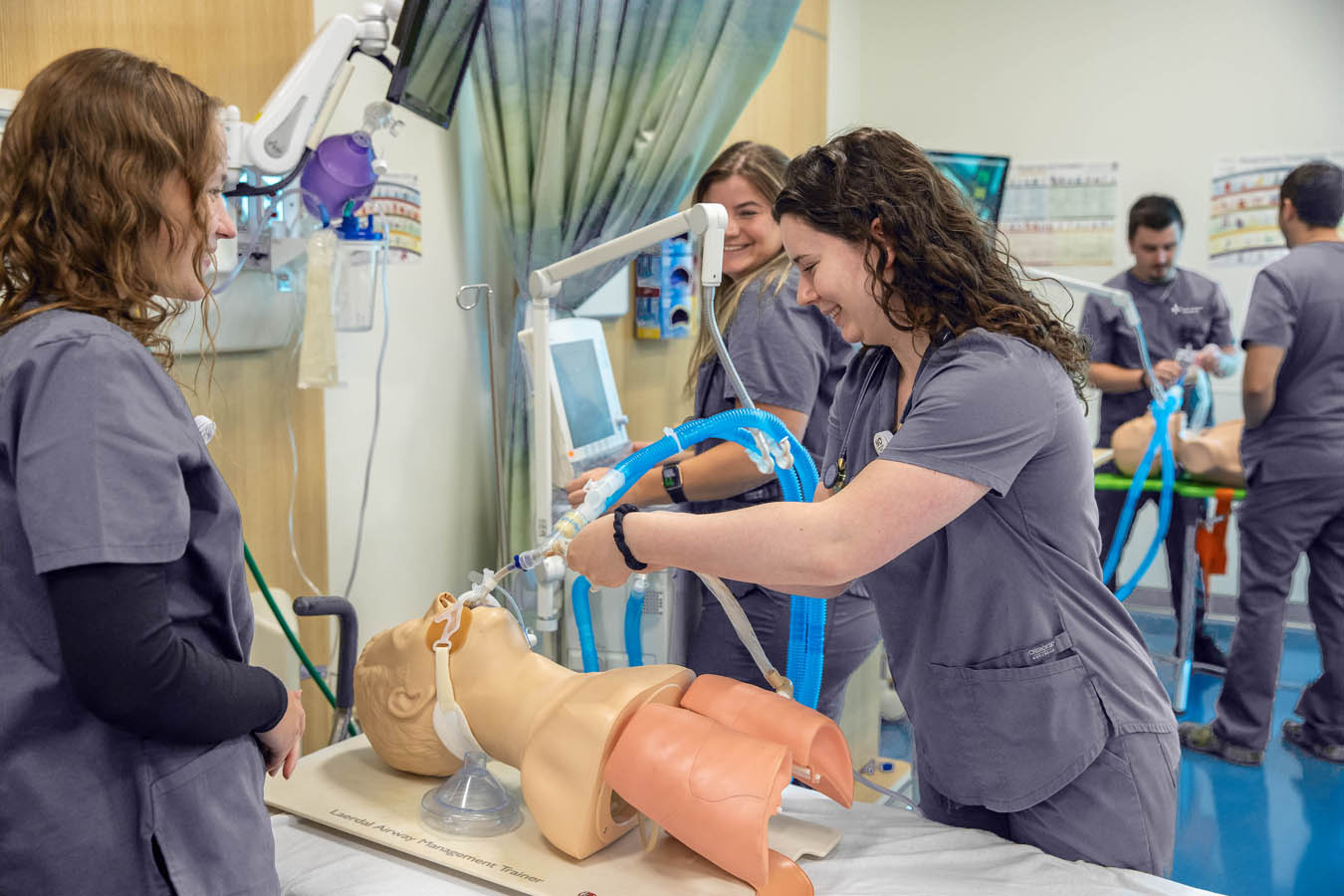
“We use pretty sophisticated respiratory manikins here,” says Best. “They have lungs that can be filled with air that can mimic a variety of different respiratory conditions.”
Students in these labs also gain practice working with ventilators that utilize pressurized gas sources to operate and gain expertise with respiratory equipment. An environment is created that mimics real-time, real-feel respiratory situations and outcomes all in a simulated setting.
“In this way, the students can manage what it’s like to have a patient with COPD or COVID,” says Best. “They get to manage those symptoms with the ventilators and react to how the scenario will change based on the ventilator settings.”
While students here primarily work on respiratory care, the space is flexible enough to be used for small-group skill practice and breakout sessions. Simulations in this lab are also viewable via camera or one-way glass.
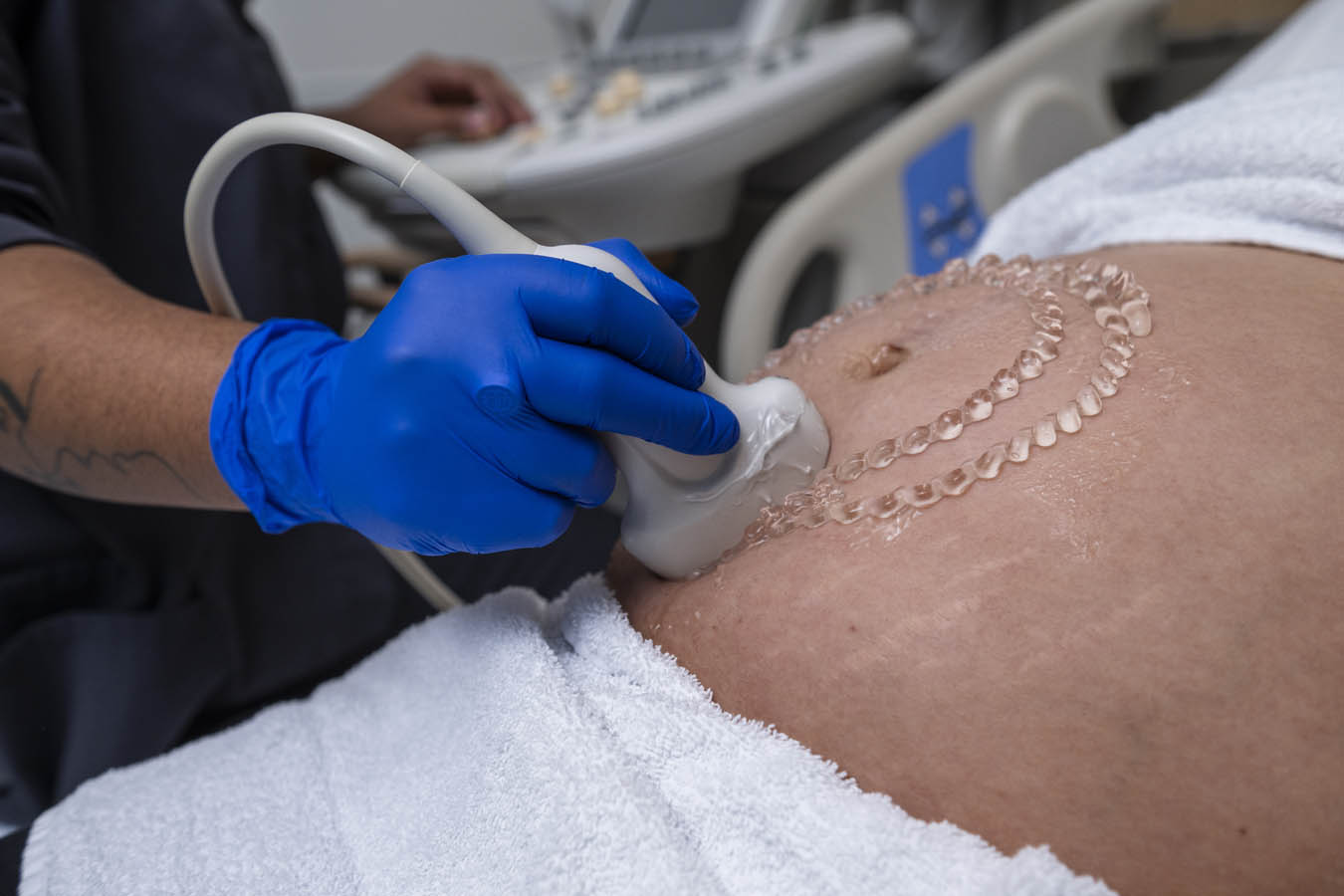
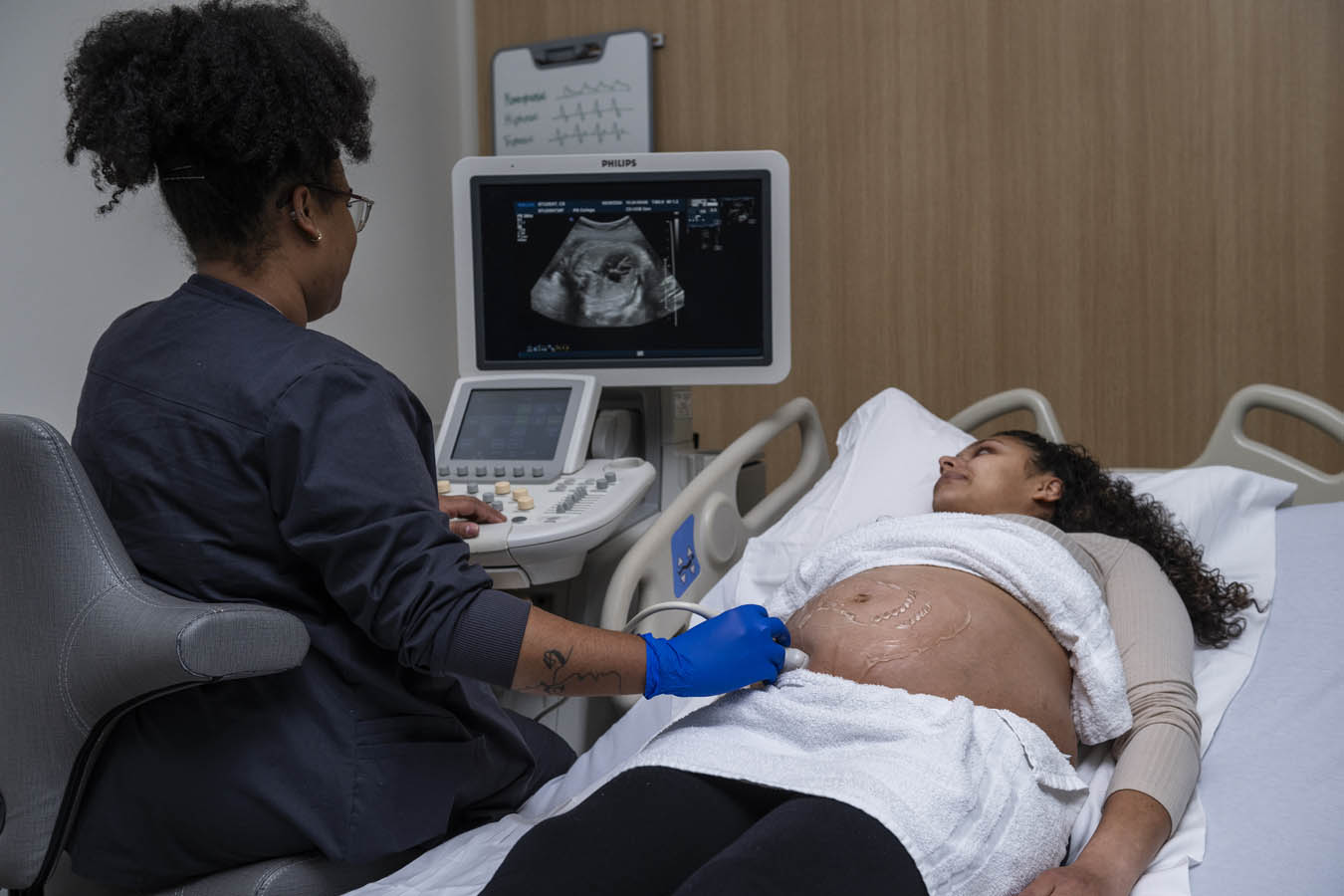
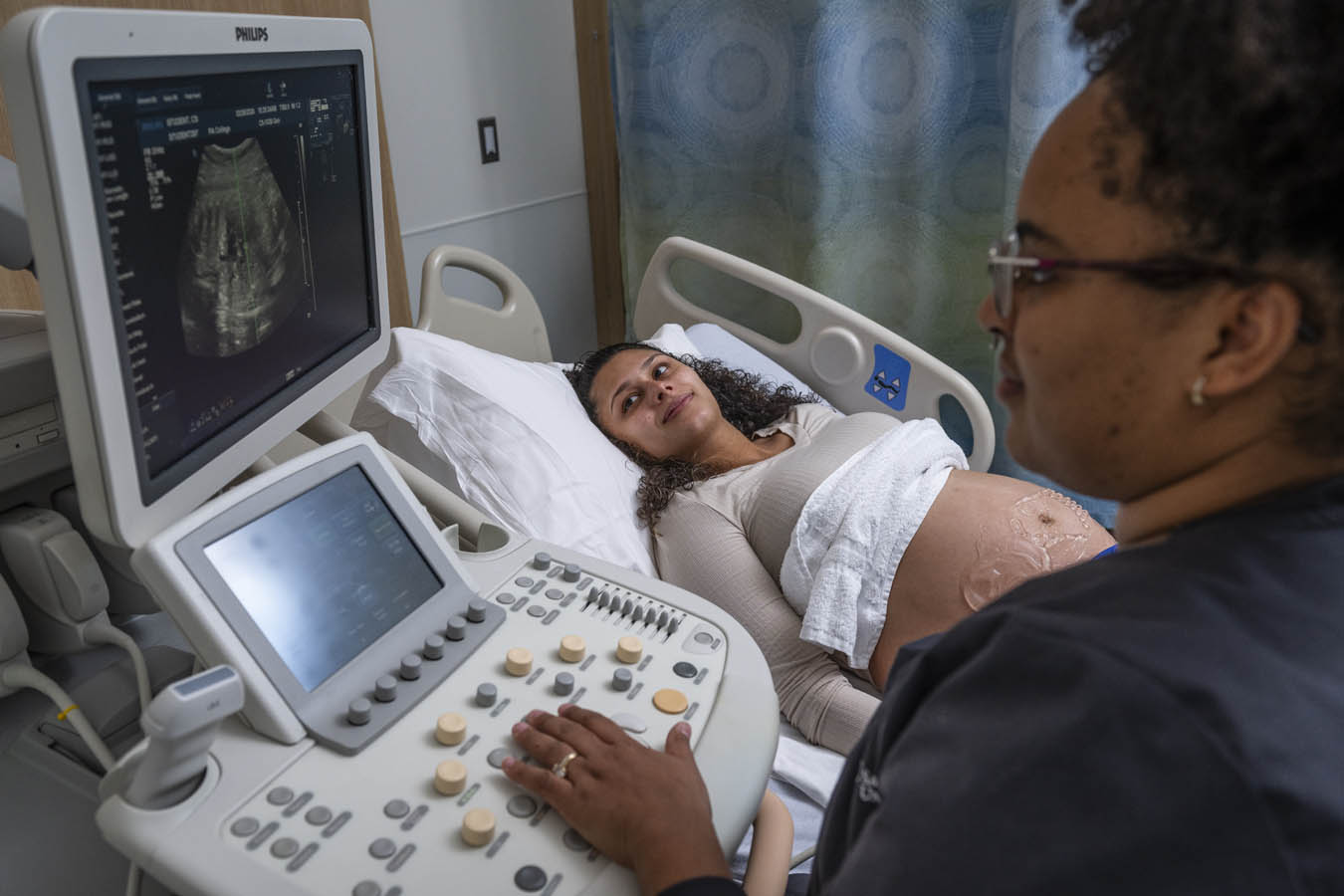
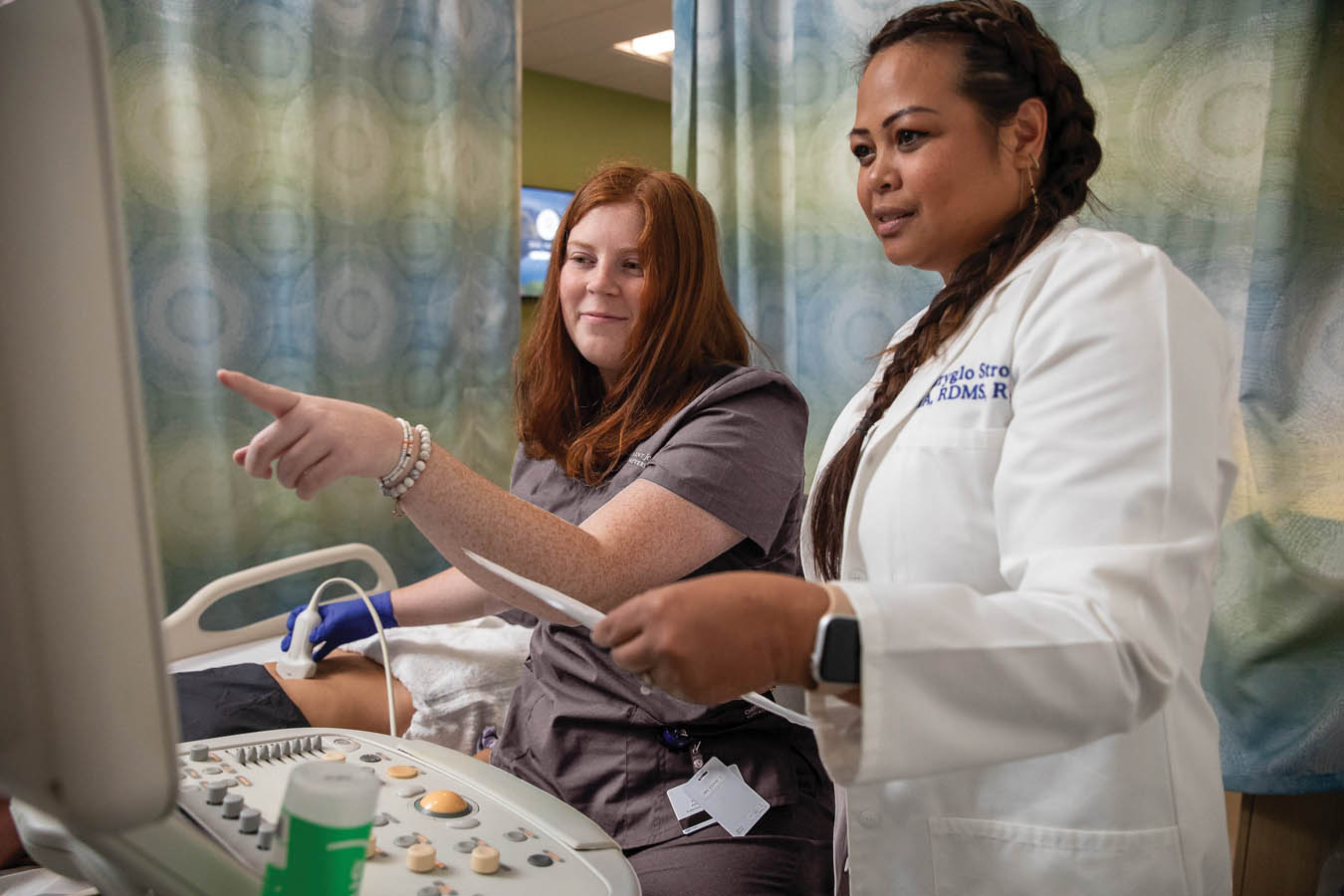
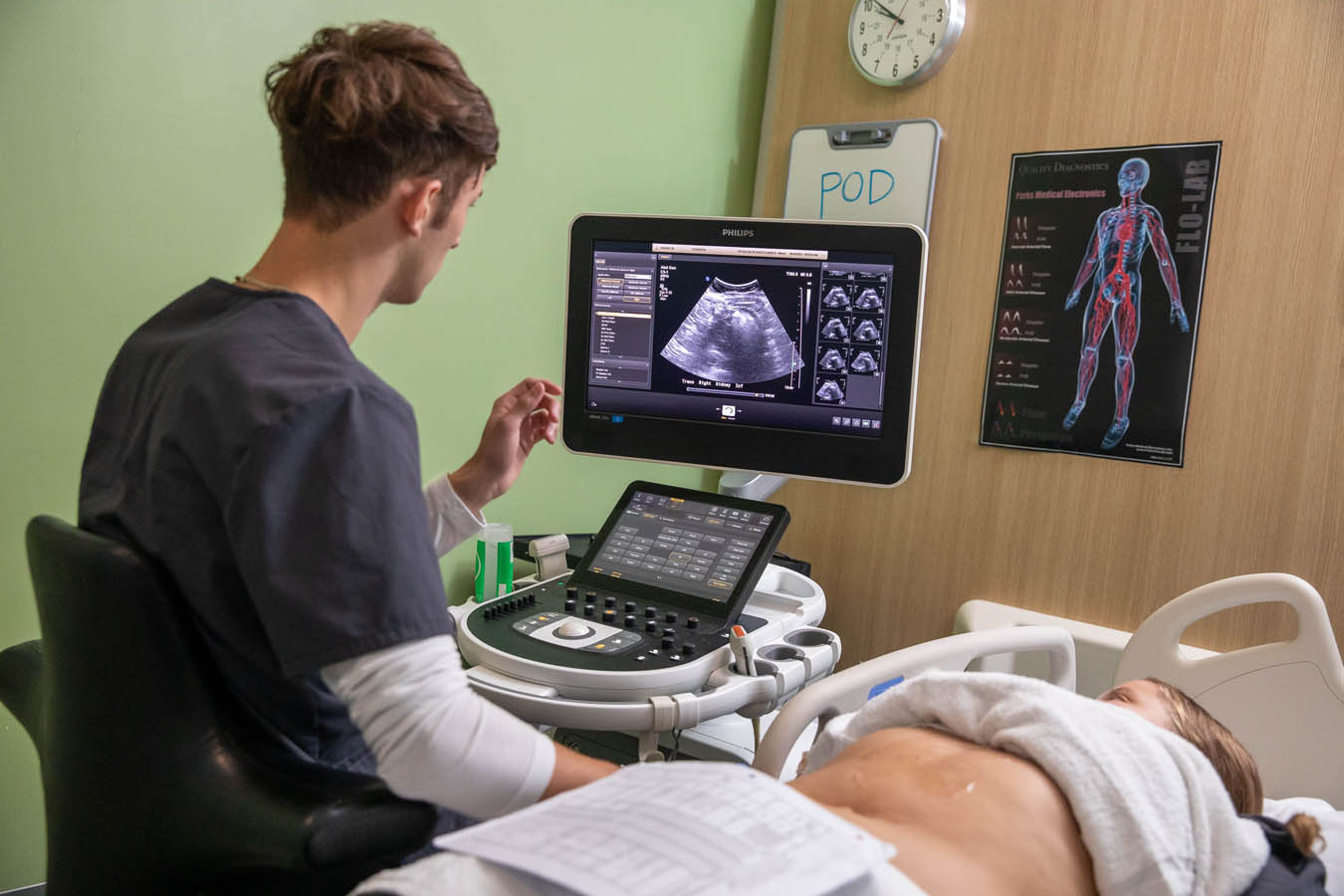
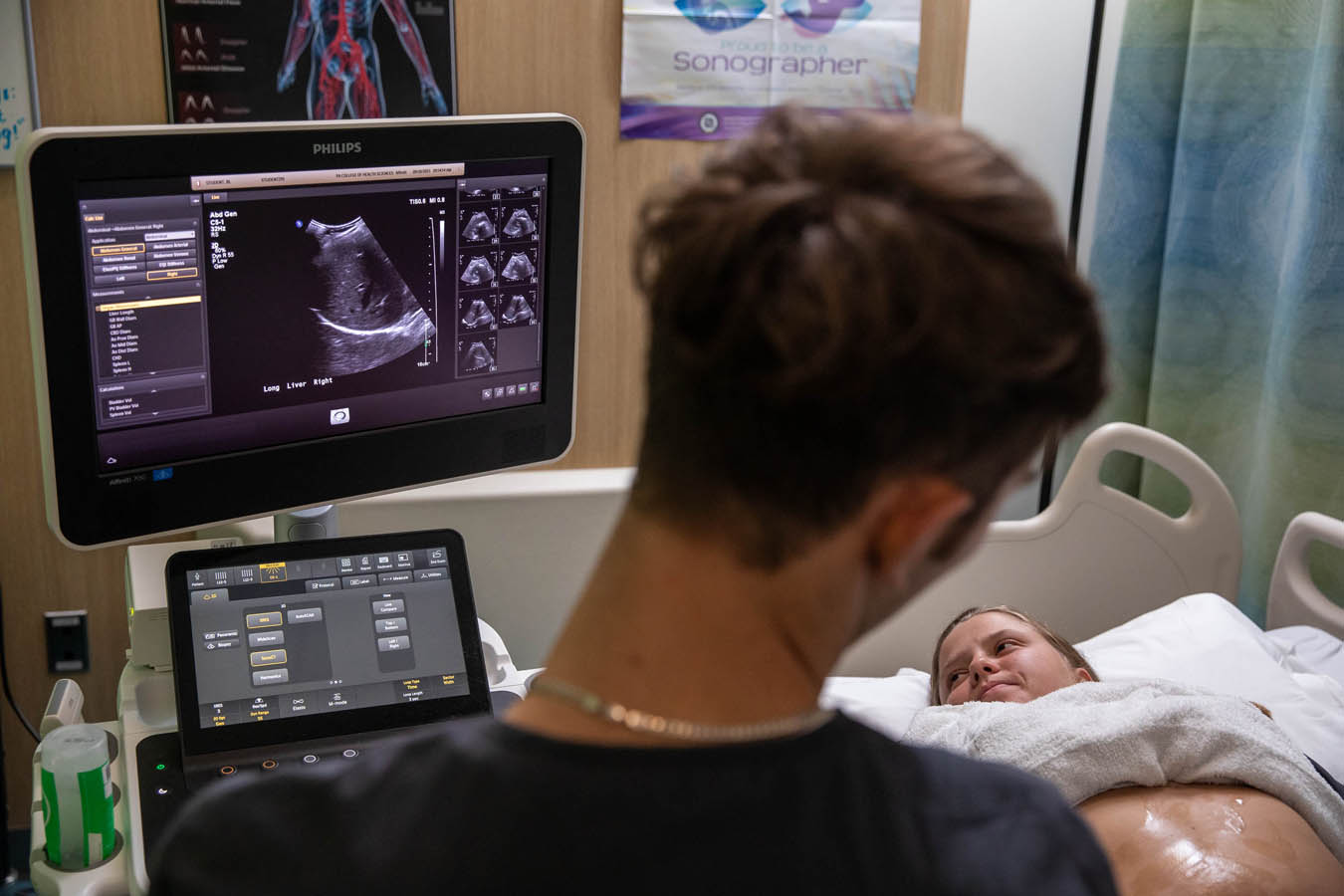
Diagnostic Medical Sonography (DMS) Lab
This lab is a flexible space, giving students access to four patient beds and a central workspace. The lab has functional sonography machines as well as virtual SonoSim modules for mid-level fidelity manikins.
Students also get hands-on experience with real-life volunteers who are pregnant or willing to get scanned. This helps students in the diagnostic medical sonography (DMS) program get a better feel for scanning real human bodies and finding particular features of internal systems.
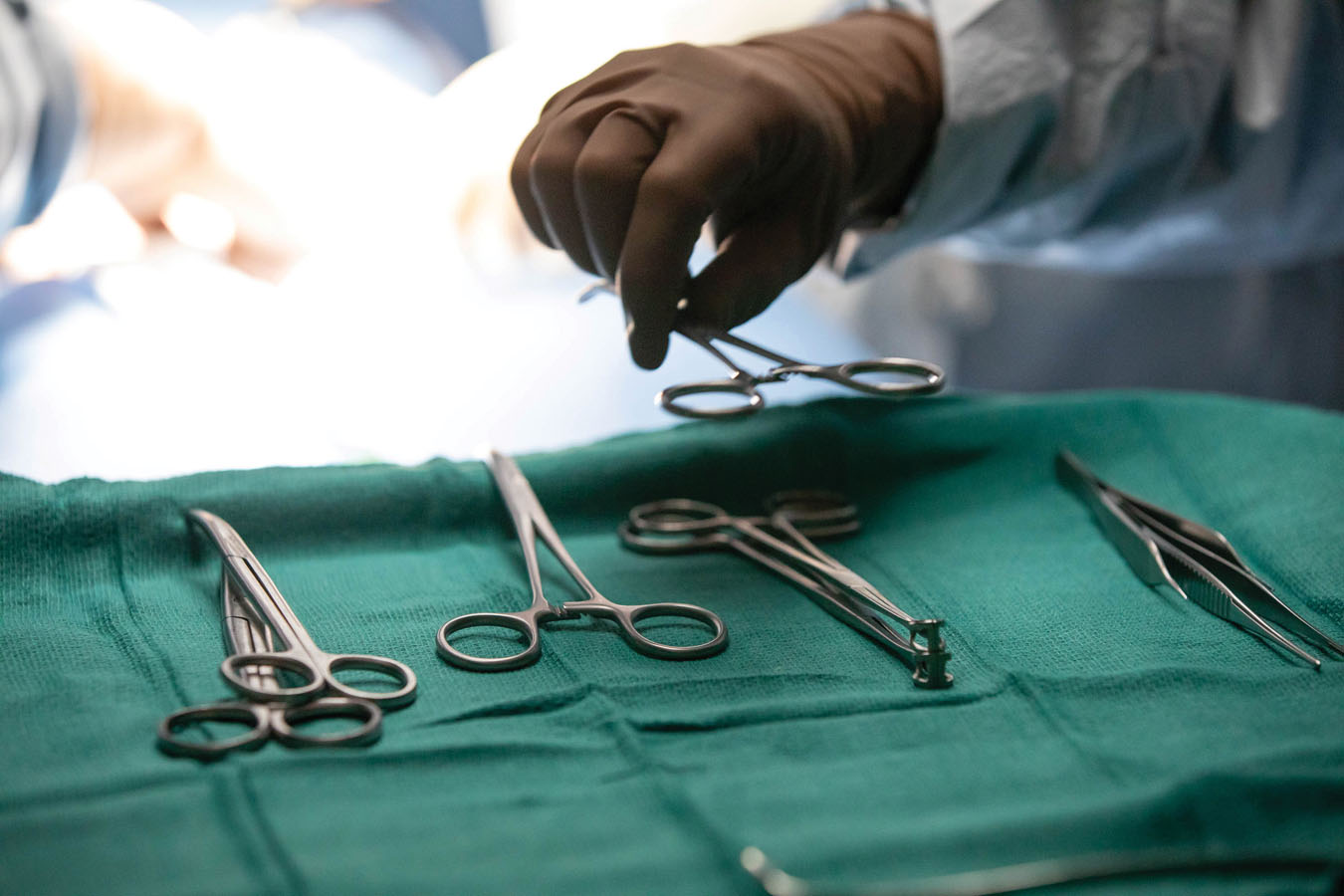
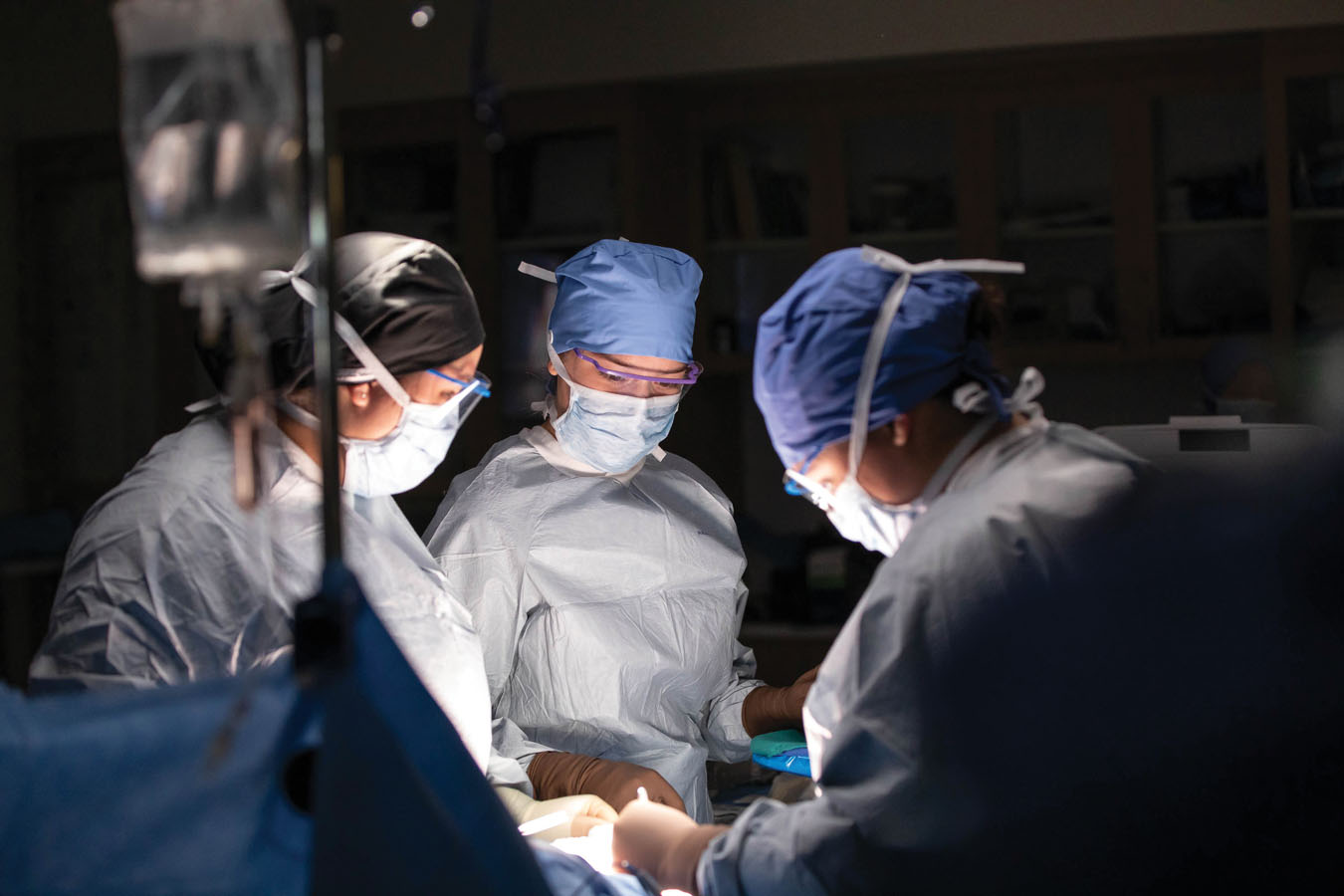
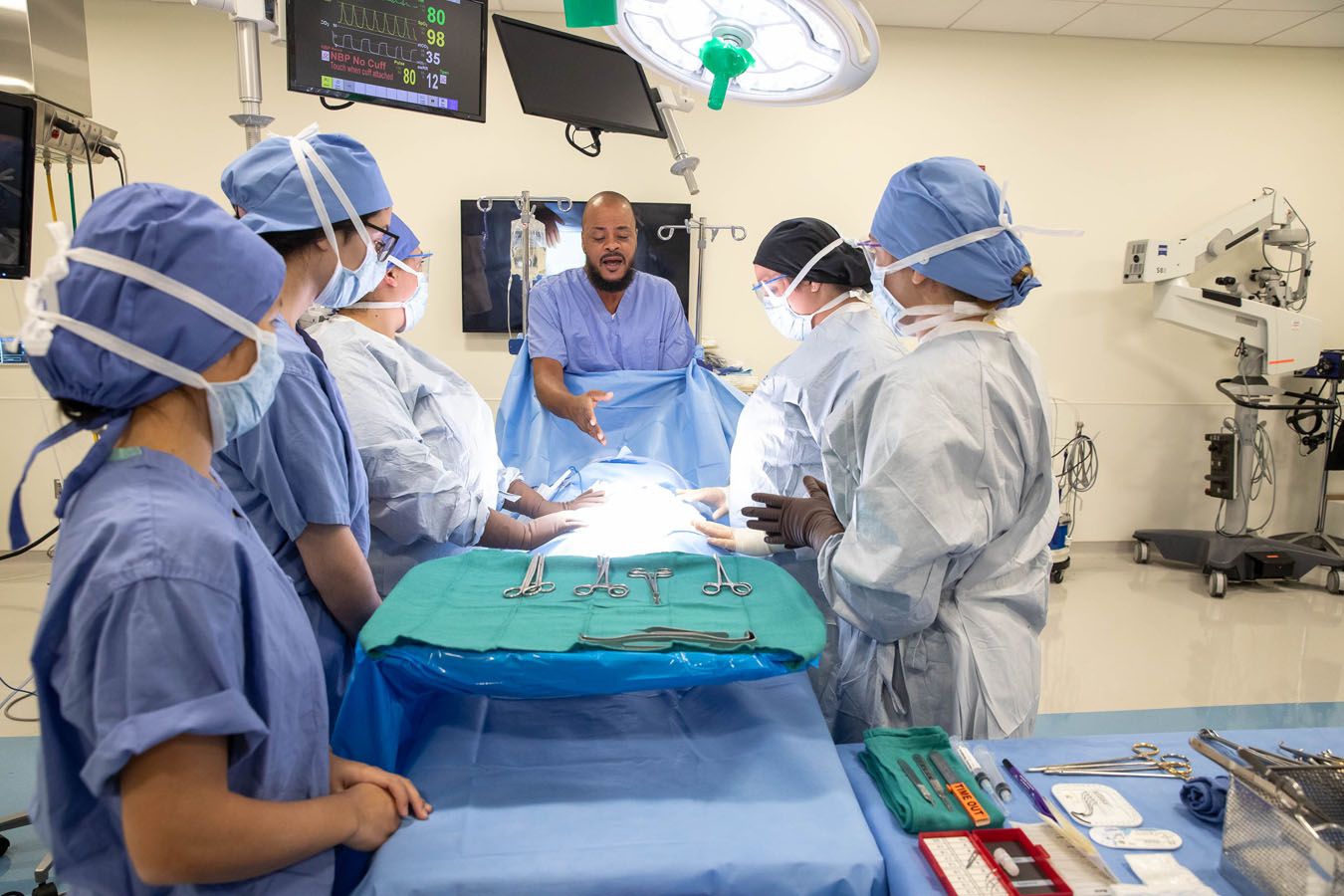
Operating Room
The CEP’s operating room (OR) features ceiling-mounted surgical lighting and monitors, retractable gas columns, and equipment booms. The space also has a functional patient table and numerous equipment trays and stands, as well as an anesthesia machine for functional gasses. Outside, students practice surgical prep with a real scrub sink.
“Surgical tech students need to be intimately familiar with tools and equipment, setting up the OR and prepping stations for surgeons,” says Zulkosky. “Patient interaction isn’t the goal here. Surg techs are much more concerned with maintaining a sterile environment, getting the right equipment, doing their surgical counts. These are the things that really matter when they’re in action.”
This unit is equipped with cameras for remote viewing, where students at work can be observed directly from the control room via one-way glass.
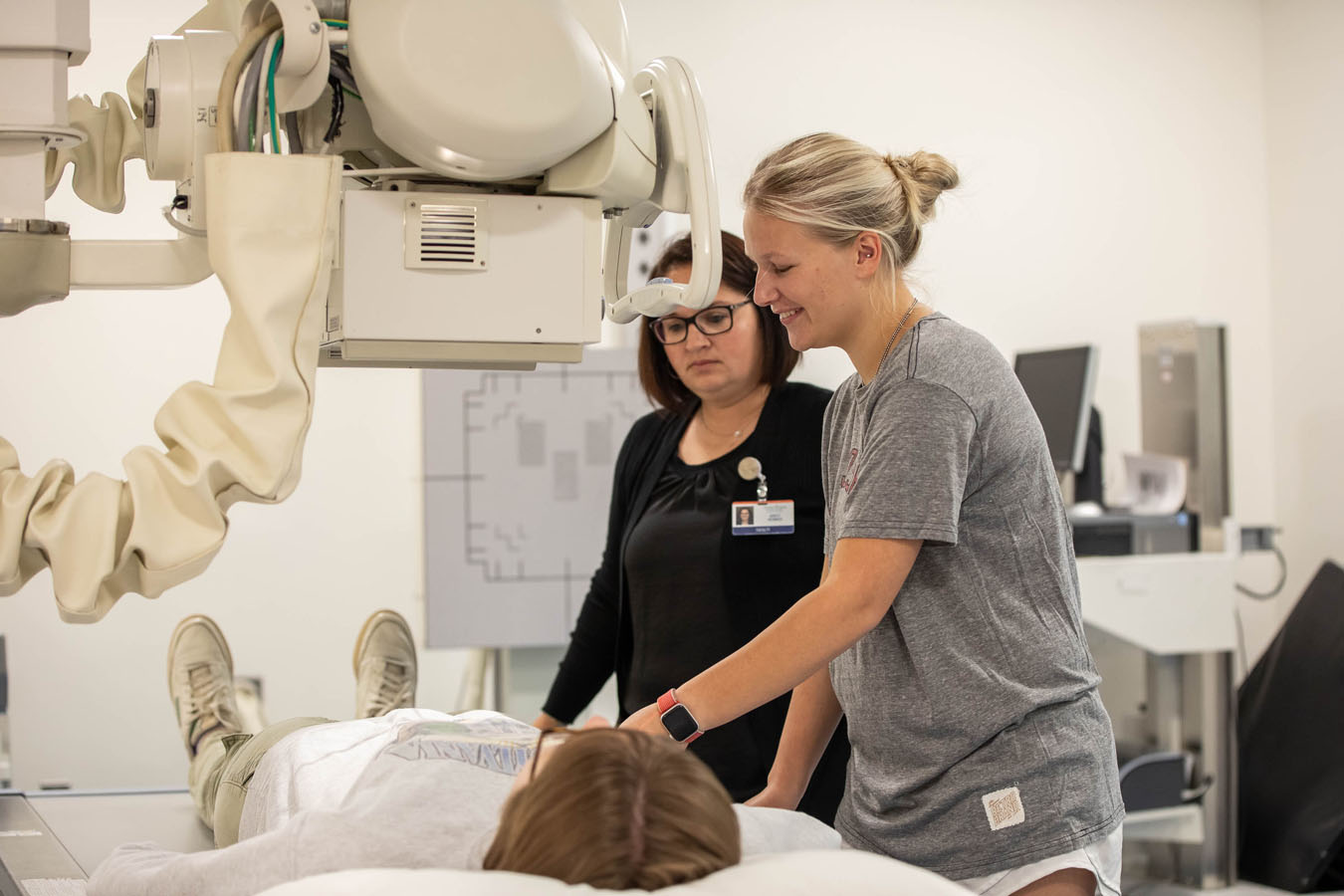
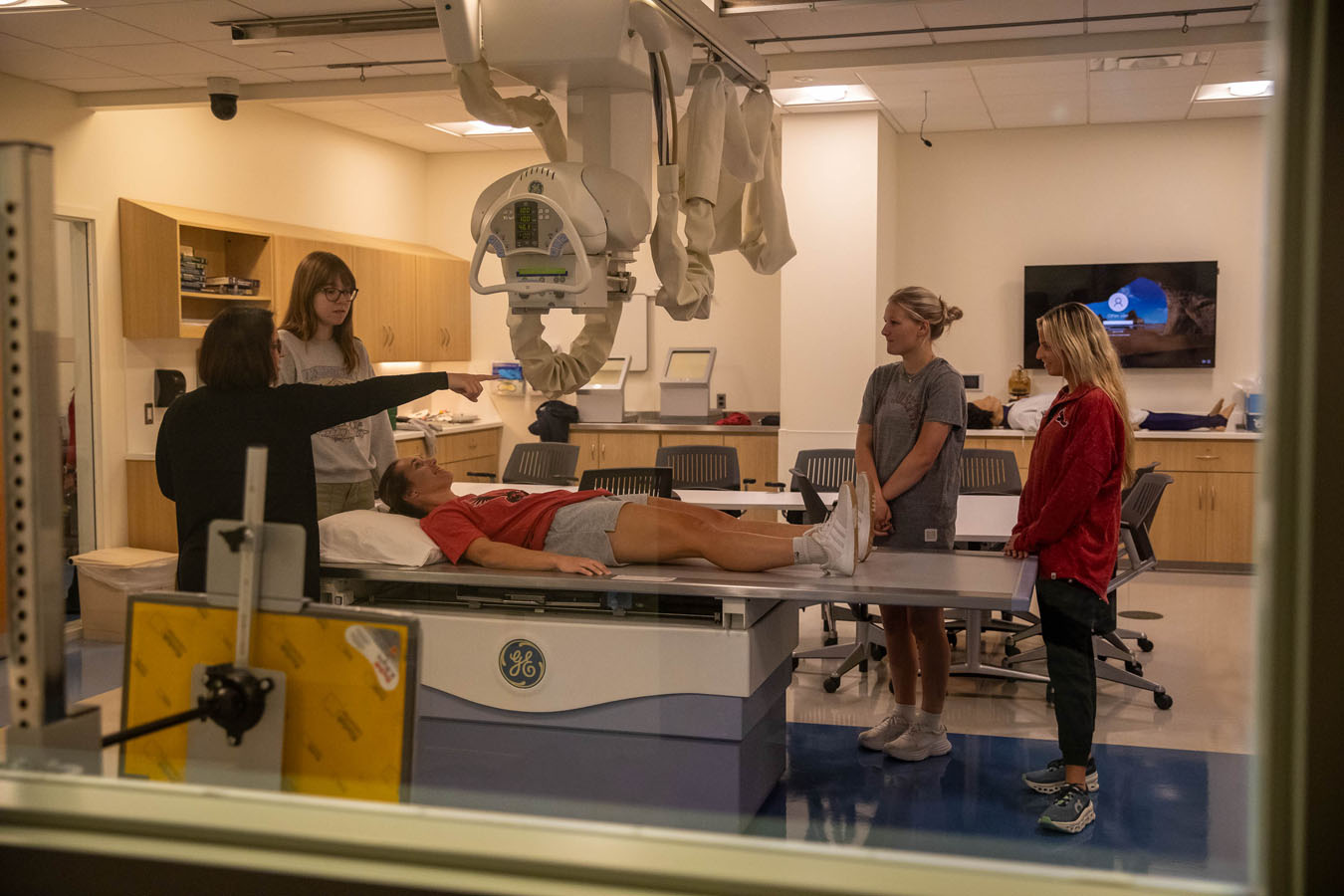
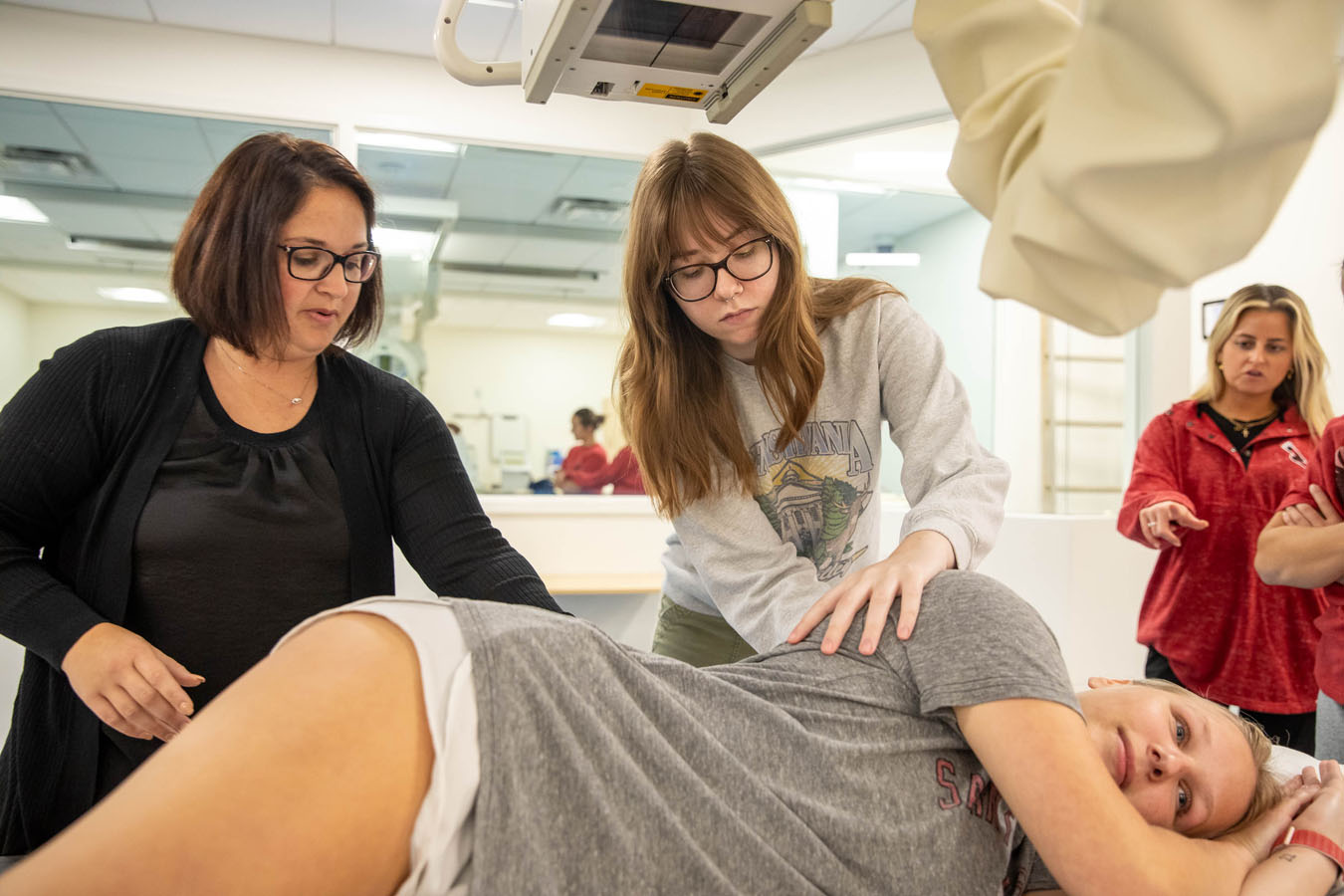
X-Ray and Nuclear Medicine Lab
Situated next to the operating room is an X-ray and nuclear medicine lab designed around an actual X-ray machine that moves and functions without live radiation.
Here, students are tested with simulated patient actors, working on properly positioning them for a variety of challenging X-ray scenarios.
The lab includes a booth for an X-ray technician and a faux “hot lab” where nuclear medicine students practice the delivery, storage and preparation of radioactive materials required for diagnostic imaging and radiotherapy.
Students learning in the CEP are rapidly gaining skills, both operationally and interpersonally, as they take on simulations where they not only relate to their patients, but also their fellow providers. In fall 2025, Saint Joseph’s will be partnering with Philadelphia College of Osteopathic Medicine to introduce an 11,000-square-foot, state-of-the-art simulation and skills lab space for Hawk Hill-based nursing students, making this kind of immersive learning experience possible for all Hawks.